Immunotherapy To Treat Cancer.
Uncategorized February 26, 2020, Comments OffImmunotherapy is a type of cancer treatment that stimulates the body’s natural defenses (immune system) to fight cancer. The immune system, when competent, helps the body fight infections and other diseases. It is composed of white blood cells, organs and tissues of the lymphatic system.
Immunotherapy is a type of biological therapy, which uses substances produced by living organisms to treat cancer. It is not yet used as much as surgery, chemotherapy and radiotherapy. However, immunotherapies have been approved to treat people with many types of cancer. Immunotheraphy has been recent in India. It is an expensive treatment but however, immunotherapy for cancer in india is being increasingly used as it provides another path for a patient to receive treatment when other options seem to fail. Compared to other countries it is less expensive in India. Immunotheraphy treatment cost can range anywhere between ₹ 1,50,000 ($2,091) – ₹4,55,000 ($6500) per session.
What are the types of immunotherapy?
The types of immunotherapy that help the immune system act directly against cancer are:
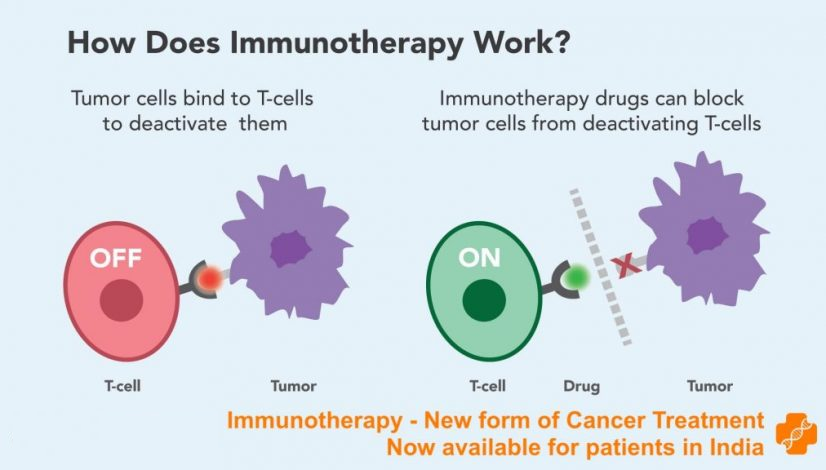
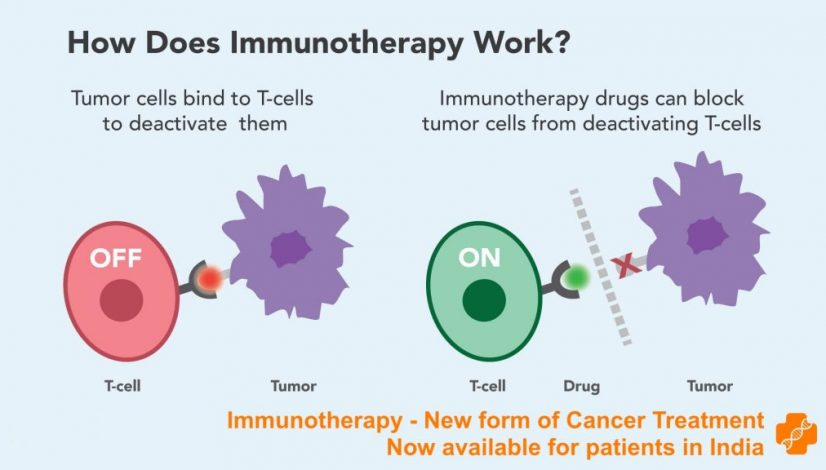
Control point inhibitors, which are drugs that help the immune system respond more strongly to a tumor. These drugs work by releasing the “brakes” that stop T cells (a type of white blood cell and a component of the immune system) so they don’t destroy cancer cells. These drugs do not attack the tumor directly. Rather, they interfere with the ability of cancer cells to evade the attack of the immune system.
These pathways are often called immune checkpoints. Many types of cancer use these pathways to evade the immune system. The immune system responds to cancer by blocking these pathways with specific antibodies called immune control point inhibitors. Once the immune system is able to find cancer and respond to it, it can stop or slow the growth of cancer.
The following are examples of inhibitors of immune control points:
- Ipilimumab (Yervoy).
- Nivolumab (Optional). Indicated for rectal colon cancer.
- Pembrolizumab (Keytruda). To treat metastatic tumors or tumors that cannot be treated with surgery.
- Atezolizumab (Tecentriq).
- Avelumab (Bavencio).
- Durvalumab (Imfinzi).
Adoptive cell transfer, which is a treatment that tries to strengthen the natural ability of your T cells to fight cancer. In this treatment, T cells are taken from the tumor. Then, those that are most active against your cancer are grown in large batches in the laboratory.
The process of growing the T cells in the laboratory can take 2 to 8 weeks. During this time, you can receive treatments such as chemotherapy and radiotherapy to reduce immune cells. After these treatments, the T cells that were grown in the laboratory will return to the body through a needle in the vein. The use of T cells for therapy has been very effective in the treatment of certain blood cancers. Researchers are still studying this and other ways to modify T cells to treat cancer.
Monoclonal antibodies, also known as therapeutic antibodies, which are immune system proteins created in the laboratory. These antibodies are designed to adhere to specific targets found in cancer cells. Some monoclonal antibodies mark cancer cells so they can be seen more easily and destroyed by the immune system, these are a specific type of immunotherapy. Other monoclonal antibodies used in cancer treatment do not cause an immune system response.
Treatment vaccines, which work against cancer by reinforcing the reaction of your immune system to cancer cells. Treatment vaccines are different from those that help prevent disease.
Types of non-specific immunotherapy, which improve the body’s immune response to fight cancer are:
Cytokines, which are proteins produced by the body’s cells. They have important functions in the body’s normal immune responses, and in the ability of the immune system to respond to cancer. The two main types of cytokines used to treat cancer are interferons and interleukins.
Oncolytic virus therapy uses genetically modified viruses to kill cancer cells. First, the doctor injects a virus into the tumor. Then, the virus enters the cancer cells and reproduces. As a result, cells explode and die. As cells die, they release specific substances called antigens. This causes the patient’s immune system to target all cancer cells in the body that have those same antigens. The virus does not enter healthy cells.
Bacillus Calmette-Guérin, BCG, is an immunotherapy used to treat bladder cancer. It is a weakened form of the bacteria that causes tuberculosis. When inserted directly into the bladder with a catheter, the BCG causes an immune reaction against cancer cells. It is also being studied in other types of cancer.
How does immunotherapy against cancer work?
One reason why cancer cells thrive is because they are able to hide from the immune system. Certain immunotherapies can mark cancer cells to make it easier for the immune system to find and destroy them. Other immunotherapies strengthen the immune system so that it works better against cancer.
Immunotherapy can work:
- By stopping or delaying the growth of cancer cells.
- By preventing cancer from spreading to other parts of the body.
- By helping the immune system to work better when it destroys cancer cells.
What are the side effects of immunotherapy?
Sometimes, immunotherapy causes the immune system to attack healthy cells, which can cause side effects.
The side effects of immunotherapy can be mild, moderate or even life-threatening. Depending on the severity of the side effects, the doctor may stop treatment or prescribe a type of medicine called a corticosteroid. If the side effects worsen or do not improve, the doctor may stop the immunotherapy.
The side effects will depend on the degree of health the patient has before receiving treatment, on their type of cancer, on how advanced they are, on the type of therapy you receive, on the dose and on other underlying diseases such as, for example, diabetes or hypertension.
The most common side effects are skin reactions at the needle site. These side effects are:
- Pain.
- Swelling.
- Irritation.
- Redness.
- Itching.
- Rash.
Symptoms such as:
- Fever
- Shaking chills
- Weakness
- Dizziness
- Nausea or vomiting
- Muscle or joint pain
- Tiredness
- Headache
- Difficulty breathing
- Low or high blood pressure
Other side effects may be:
- Swelling and weight gain due to fluid retention
- Heart palpitations
- Sinus congestion
- Diarrhea
- Risk of infection
Immunotherapies can also cause severe or even fatal allergic reactions. However, these reactions are rare.
How is immunotherapy given?
Different forms of immunotherapy can be administered in different forms. These are:
-
Intravenous (IV)
Immunotherapy is given directly into a vein.
-
Oral
Immunotherapy is given in tablets or capsules to be taken by mouth.
-
Topical
Immunotherapy has a cream that is applied to the skin. This type of immunotherapy can be used for skin cancer, very early on.
-
Intravesical
Immunotherapy is given directly into the bladder.
How often is immunotherapy received?
How often and for how long immunotherapy is received, will depend on:
- Type of cancer and how advanced it is.
- The type of immunotherapy you receive.
- How the body reacts to treatment.
You may receive treatment every day, once a week or once a month. Some immunotherapies are given in cycles, a cycle is a period of treatment followed by a period of rest. The rest period gives the body the chance to recover, react to immunotherapy and produce new healthy cells.
The future of cancer immunotherapy.
As knowledge about the immune system and the biology of tumors increases, the hope for developing treatments that can change people’s lives grows.
Great progress has been made in recent years, with immunotherapies that point to specific aspects of certain tumors.
The combination of different treatments, which in some cases is already being carried out, will allow even greater progress.
Immunotherapy for cancer represents an exciting and evolving area of research.
Knowing in depth the immune biology, knowing how to strengthen it and achieve an immune response against cancer, could definitely change the way you think about this disease and its treatment in the near future.